
More patients are seeking medical care outside of the United States for procedures ranging from cosmetic surgery to dental work and fertility treatment, and Black patients are among those driving this shift. While clinicians may be inclined to discourage international care due to safety concerns, many patients make these decisions based on cost, access, and a desire for a more respectful and culturally comfortable experience.
Rather than resisting the trend of medical tourism, providers are in a position where they understand where patients are going, why they are leaving, and how to support them before and after treatment. Insights from Charlisa D. Gibson, MD, a critical care and pulmonary physician at UM Baltimore Washington Medical Group and Assistant Treasurer for the Friends of the Public Hospitals Authority of the Bahamas, offer a practical framework for clinicians navigating these conversations while prioritizing patient safety and continuity of care.
Patients are not choosing destinations randomly; instead, they are selecting countries known for specific types of care combined with lower costs. Dr. Gibson says people she sees are heading to Cuba for overall medical care, Brazil for plastic surgery, and Barbados for fertility treatments.
Cost is the primary driver for most patients. However, other Black patients are choosing Canada and Mexico for lower-cost routine procedures, when driving conditions permit. And others are going to predominantly Black countries like South Africa or Muslim-majority countries like Turkey, when culture and religion factor into destination decisions.
These patterns reflect both specialization and affordability, with certain countries building reputations in specific fields. For providers, understanding these trends helps contextualize patient decisions and anticipate the type of care patients may receive abroad. It also allows clinicians to move beyond general warnings to provide targeted, relevant guidance tailored to the destination and procedure.
The types of procedures patients seek abroad often highlight gaps in domestic access and affordability. Dental care, fertility treatments, and elective cosmetic surgeries are among the most common categories. Dr. Gibson says cost is the primary driver, underscoring that many of these procedures are not covered by insurance, often making international care the only viable option.
Clinicians should be careful not to appear judgmental when approaching conversations with patients, as many feel that traveling abroad may be the only way to address their concerns.
Instead, providers could help patients make an informed decision, considering other factors outside of location, such as:
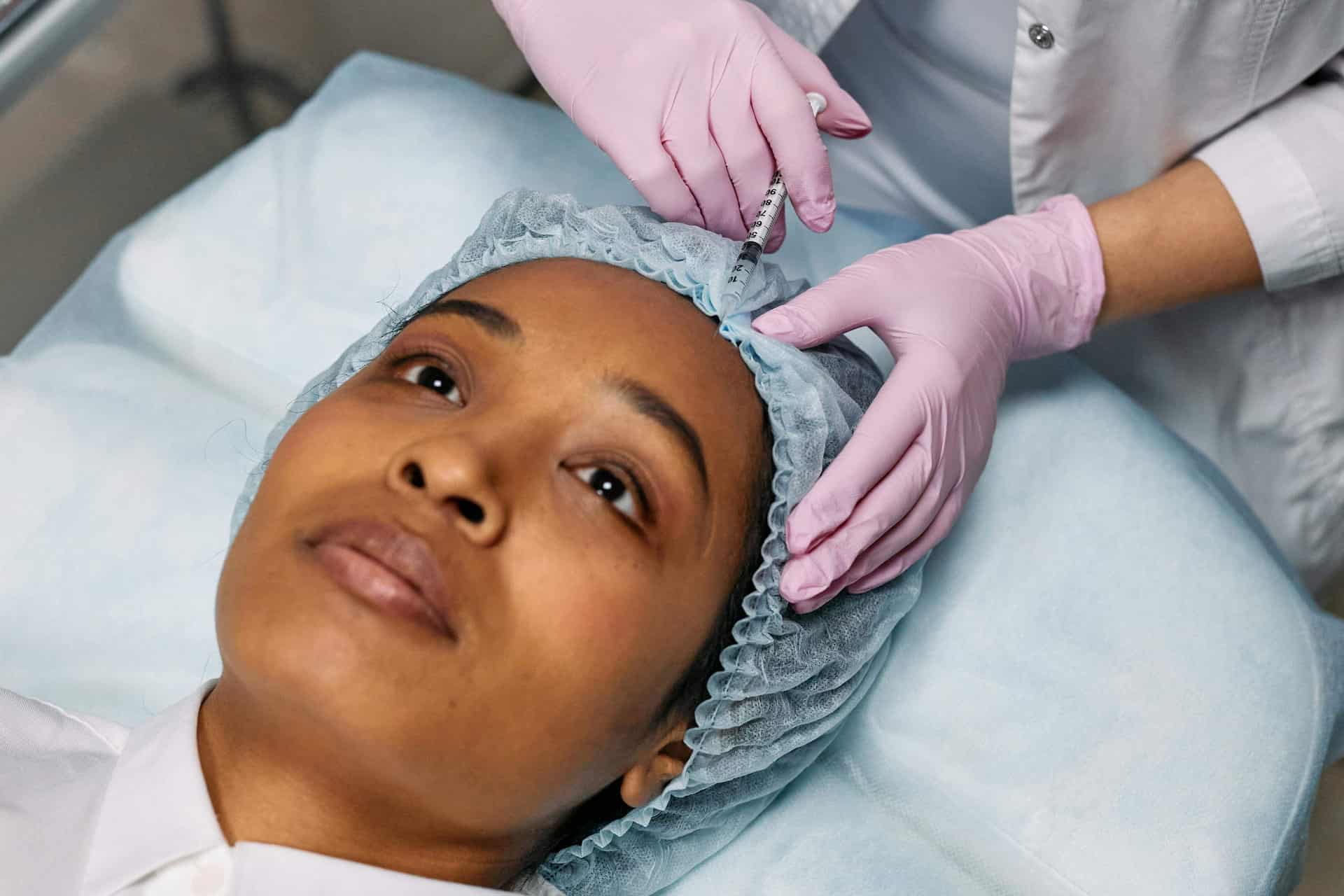
Dr. Gibson notes that “from what patients express to me, cost and a desire not to be marginalized in bigger health systems significantly contribute to seeking care outside of the US.” When patients feel dismissed or underserved, they may seek care in environments where they believe they will be treated with greater dignity and attention. Similarly, physician credentials are now readily available online, making it easier to shop around for the best possible care globally rather than locally.
For immigrant-heritage families, the option of going elsewhere may be even more accessible. They may travel to a place with extended family support, personal experience with a trusted family physician, or linguistic familiarity, which may ease concerns about getting a procedure in the first place.
For providers, medical tourism may seem like competition, but in many cases, it is not. The best approach is to create space for honest dialogue, as these relational factors can directly influence whether patients share their plans and whether they return to a provider for care.
Discouraging medical tourism outright can damage the patient-provider relationship, particularly in communities where medical mistrust already exists. Dr. Gibson explains that “it is often counterproductive to discourage medical tourism because of the history of medical mistrust in the U.S.
Amongst people of color, for diagnoses like cancer and asthma, Black patients have worse health outcomes and increased mortality.” Instead, Dr. Gibson advises “asking open-ended questions to understand patient reasons for seeking care outside of their home country and offering help/guidance every step of the way.” This approach allows providers to remain involved in the patient’s care journey while still addressing potential risks.
Continuity of care is critical when patients return from international treatment, particularly if complications arise or new medications are involved. Dr. Gibson emphasizes the importance of early follow-up, stating that providers should focus on “ensuring medical reconciliations are thoroughly done at the first visit following their return, ideally within the first two weeks.”
According to the London Health Sciences Centre, medical reconciliations (Med Rec) are the “process of comparing a patient’s medication and drug dose history to his or her current medications. This is done to prevent accidental disruption of important medications or drug dose errors.”
Medical reconciliations help identify discrepancies, prevent adverse interactions, and ensure appropriate follow-up care, wherever the patient goes. Providers can also prepare patients before they travel by encouraging them to keep detailed records of their procedures and treatments.
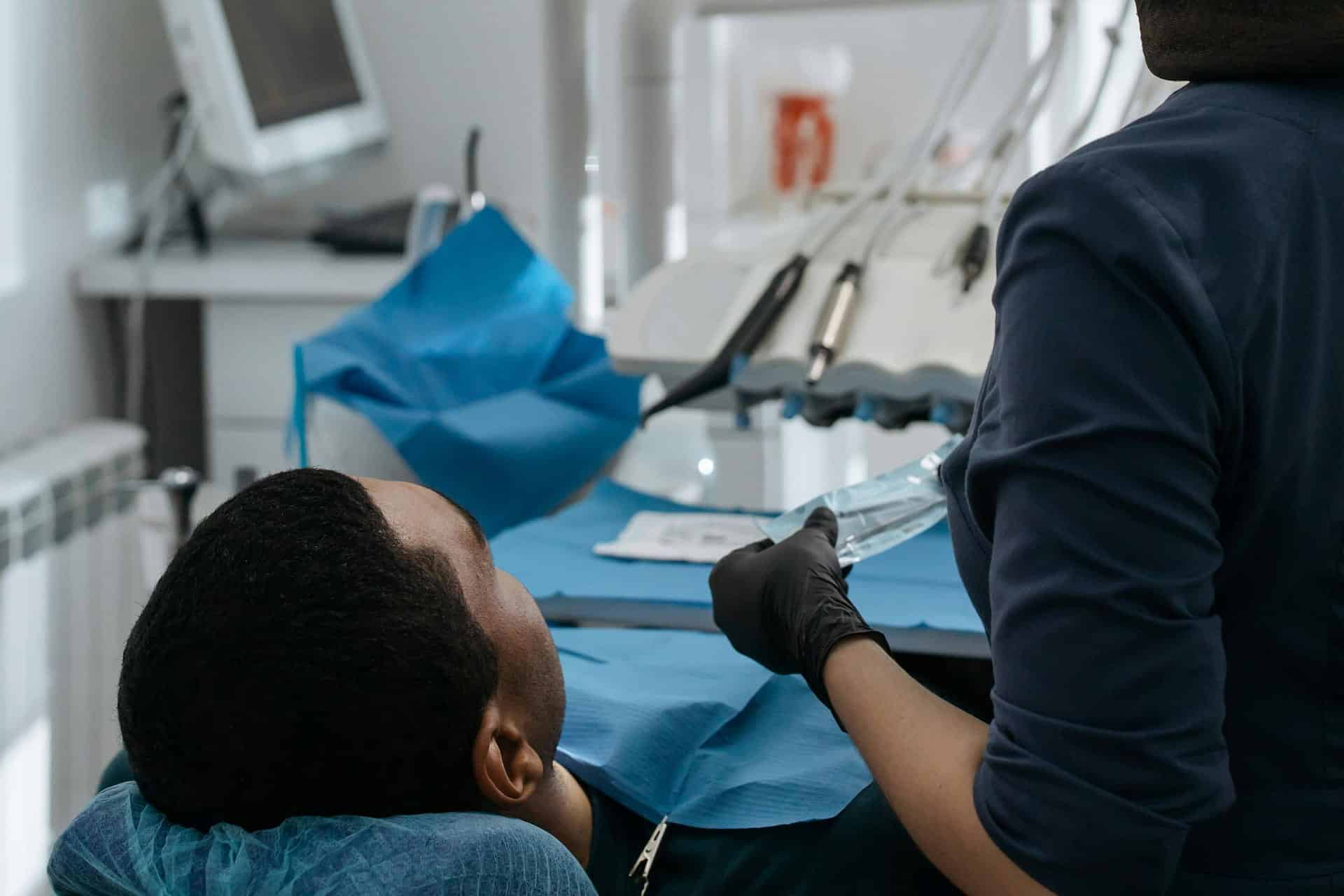
Thanks to social media influencers and higher out-of-pocket costs for cosmetic procedures, medical tourism will continue to rise among Americans. By taking a proactive, supportive approach, clinicians can reduce risks and ensure that patients who pursue care abroad return safely and receive coordinated care upon return home.
By subscribing, you consent to receive emails from BlackDoctor.pro You may unsubscribe at any time. Privacy Policy & Terms of Service.
Are you a healthcare professional? Register with us today!