
Cardiovascular disease remains the leading cause of death in the United States — claiming over 940,000 lives yearly — but the outcomes differ among racial and ethnic groups. Black Americans, in particular, face higher rates of cardiovascular disease, hypertension, stroke, and heart failure — and lower survival rates after cardiac emergencies.
New data from the American Heart Association’s (AHA) 2026 Heart Disease and Stroke Statistical Update highlights a persistent gap in CPR education and bystander response in Black communities, reinforcing the need for healthcare professionals to engage in culturally responsive training and outreach.
Cardiac arrests that occur outside of hospital facilities affect more than 350,000 Americans annually, yet the survival rates remain low, largely due to immediate CPR not being administered in most cases. Performing immediate CPR can double or triple the chances of survival.
Yet, many studies show that Black victims of cardiac arrest are less likely to receive bystander CPR at home than white people.
This disparity arises from several factors, including:
The latest data from the AHA underscores the broader cardiovascular disparities affecting Black Americans:
These disparities emphasize the need for better emergency medical response among communities facing a higher cardiovascular risk.
The minutes that follow a cardiac arrest are the most critical, as brain injury can develop within four to six minutes without oxygen. Survival often depends more on bystander intervention than on emergency responders.
“In a cardiac emergency, the first few minutes belong to the people nearby, not the hospital,” said William “BJ” Hicks II, MD, a vascular neurologist specializing in stroke treatment, prevention, and research, to the AHA. “Black Americans are more likely to have their heart suddenly stop and less likely to receive lifesaving CPR or AED help. That’s why expanding Hands-Only CPR and AED awareness in Black communities is urgent. When more families, neighbors, and faith communities are trained and confident to act, more lives can be saved.”
Dr. Hicks was named the American Heart Association’s 2025 Physician of the Year for his leadership in establishing mobile stroke treatment units in his hometown of Columbus, Ohio.
Hands-Only CPR — chest compressions without mouth-to-mouth breathing — can easily be taught in minutes and significantly increase survival chances among Black Americans.
The process involves two simple steps:
Despite the straightforward process, many people are still hesitant to intervene during an emergency. In fact, surveys reveal that while Black people’s confidence in performing CPR has improved in recent years (30 percent in 2021 to 44 percent in 2023), significant knowledge gaps persist.
Healthcare providers can play a significant role in improving bystander CPR in the Black community through improved patient interactions and community outreach.
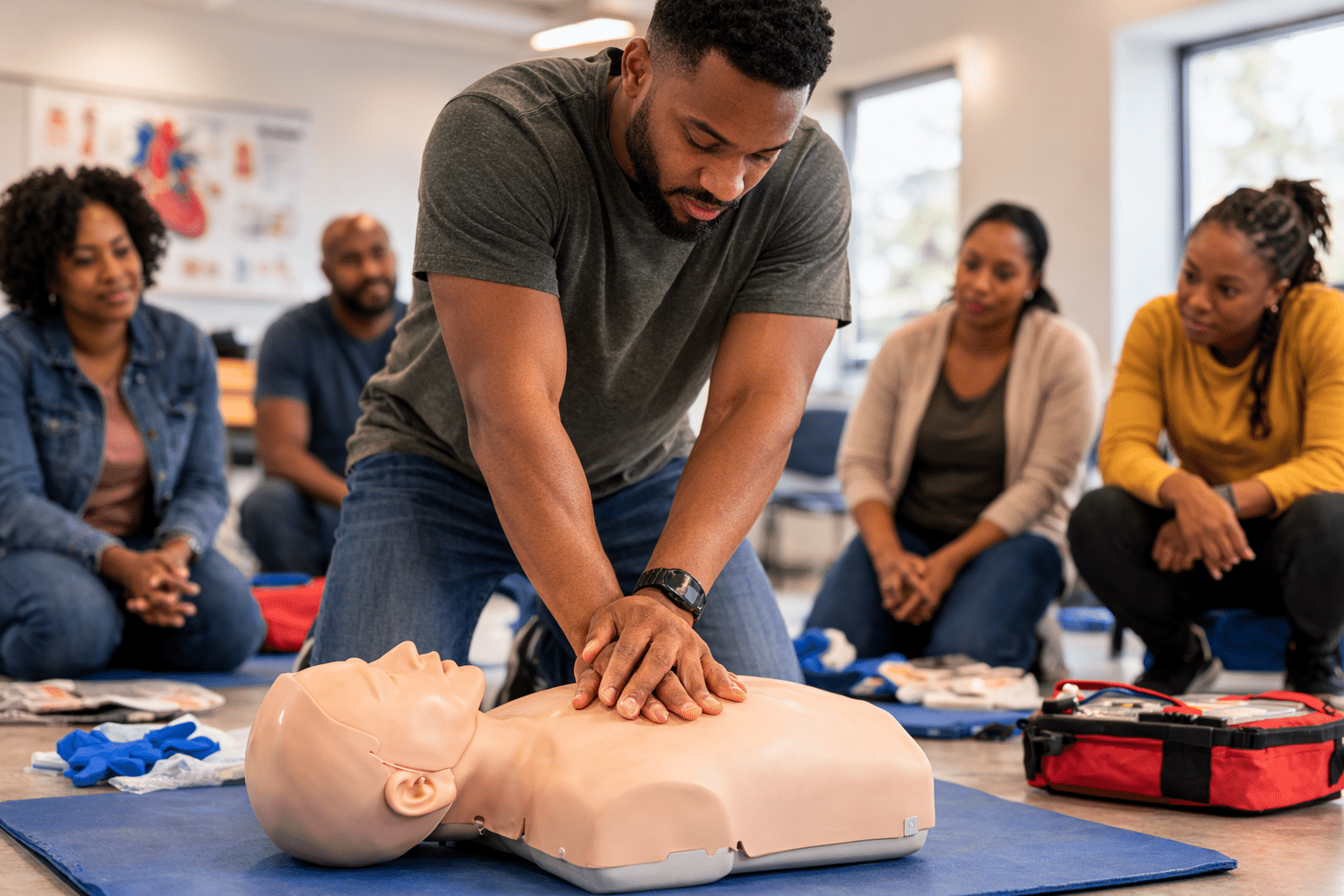
The following strategies can encourage more Black participation in CPR training and education to increase survival outcomes from cardiac arrest:
Healthcare providers can encourage better CPR training in the Black community by:
Clinicians can also consider implementing CPR education into discharge planning for patients with cardiovascular disease or those at a heightened risk of cardiac arrest.
Improving survival outcomes requires more than just medical care — it requires building community readiness.
The AHA’s “Nation of Lifesavers” initiative aims to increase bystander CPR rates across the U.S. by empowering people with the skills and confidence to respond to cardiac emergencies. The goal is to have at least one person in the household trained in CPR.
For Black Americans, expanding CPR education and training could help address long-standing disparities in emergency cardiovascular care.
When more family members, neighbors, and community members are trained to respond to cardiac emergencies, the chances of survival significantly increase before EMS arrives — leading to more lives being saved.
By subscribing, you consent to receive emails from BlackDoctor.pro You may unsubscribe at any time. Privacy Policy & Terms of Service.
Are you a healthcare professional? Register with us today!