The heart can age quicker than your years. Medical research suggests that for many Black women, biological age may outpace chronological age. The phenomenon, known as “weathering,” was coined by Arline T. Geronimus, Sc.D., to consider how chronic oppression, racism, and other hardships can change the body and affect heart health.
Her studies, and those that build upon them, indicate that Black women’s bodies can show signs of accelerated aging, including cardiovascular strain, years earlier than their white counterparts. The concept centers on allostatic load: the cumulative physiological toll of chronic stress from socioeconomic disadvantage, discrimination, and structural inequities. In other words, emotional and physical “wear and tear” can break down the body’s vital organs faster than age would indicate.
For clinicians relying solely on traditional cardiovascular risk calculators, this raises the critical concern that standard metrics can underestimate risk. Understanding biological age versus chronological age may offer providers a more comprehensive framework for guiding patient care.
What Does “Weathering Age” Mean?
At its simplest, weathering age reflects the gap between someone’s chronological age and their biological age. “Weathering age is biological minus chronological age.” In measurable terms, she notes,” explains Ashley Katzenback, PT, DPT, CMTPT. “Studies have demonstrated that African American women show biological aging that is approximately six years accelerated compared to white women, using lipid levels, glucose, inflammatory markers, and pulmonary function.”
This accelerated aging is not primarily attributed to lifestyle choices. Katzenback emphasizes that it “has been linked to neighborhood disadvantage, discrimination, and financial pressure—rather than health behaviors alone.” In other words, the body’s stress response, activated repeatedly over many years, may wear down organ systems, even when diet and exercise habits are good.
Dermatologist and internist Eleonora Fedonenko, MD, echoes this understanding from a clinical lens. She notes that Dr. Geronimus introduced the term in the early 1990s after identifying worsening health outcomes among Black women compared to white women of the same age. “The theory holds that years of living under poverty, discrimination, and social strain cause the body to go into a prolonged stress response, which breaks down cells at the molecular level,” Dr. Fedonenko explains.
How Has Dr. Geronimus’s Work Evolved?
Dr. Geronimus is a public health researcher who has spent her career advancing health equity. When she first introduced the concept of weathering in the late 1990s, it was not widely embraced. Dr. Fedonenko says that Dr. Geronimus’s findings “were initially dismissed by much of the medical community.” Over time, however, peer-reviewed research expanded the evidence supporting accelerated biological aging in marginalized populations, and then her work was more consistently referenced and revered.
Even today, Katzenback admits the framework was not on her radar initially. “I had known that chronic exposure to social and economic disadvantage leads to accelerated deterioration of physical health in African American women, but I did not realize there was a name for that phenomenon and that it has been so well studied.”
Although much of this research has been around for decades, not all healthcare professionals are reading up on it or learning how to understand (and prevent) what they’re seeing in their patients.
Also, weathering does not happen exclusively to Black women. In fact, Geronimus studied birth outcomes after Latina mothers experienced an immigration raid in 2008. Today, weathering is increasingly discussed in population health research, particularly in relation to cardiovascular disease, infant and maternal mortality, and chronic inflammatory conditions.
How Can Biological Aging Differ From Chronological Aging—and Why?
Chronological age is fixed. Biological age is dynamic. This distinction matters because stress accelerates cellular wear and tear.
“Chronological age is how old you are or how many years you have been alive,” Katzenback says. “Biological age is how old all of your organ systems are. The simplest approach to determine biological age is a composite biomarker panel using seven routine laboratory and clinical measurements: lipid levels, glucose, C-reactive protein, BMI, pulmonary function (spirometry), and mean arterial pressure.”
“Your birth certificate gives you one age, but your cells tell a different tale,” Dr. Fedonenko notes. “Biological aging is the measurement of how your body truly functions at the cellular level.” She highlights telomere shortening as one measurable mechanism. “Telomeres are the caps on the ends of your chromosomes, and chronic stress depletes your telomeres faster than time does,” she says, adding that “cortisol, which is the body’s primary stress hormone, contributes to systemic inflammation that causes this wear in cells to occur.”
Over the years, that inflammatory burden may increase cardiovascular vulnerability, even when traditional risk factors would indicate otherwise.
What Can Be Done to Reverse or Slow the Weathering Age?
Now that we know the phenomenon exists, the question is: can it be reversed—or at least slowed?
Katzenback says no randomized trials have directly tested whether interventions translate into improved cardiovascular or mortality outcomes in African American women specifically. “The existing evidence suggests that Vitamin D3, improvements in diet, and decreased tobacco use should slow and potentially reverse weathering age, but nothing definitive has been shown,” she says.
The important thing to remember is that lifestyle modifications may not be enough to compensate for racial disparities in biological aging, so patients and providers should start with lifestyle changes but not end there. Testing for biological markers early can help providers see just how stressed patients are, even if patients do not verbalize or show external signs of accelerated aging.
Dr. Fedonenko adds that continued access to high-quality care is critical. “In my work with patients from underserved communities, it is not information that is the barrier. It’s access to consistent, culturally informed medical care that treats the whole person.” Interventions targeting inflammation and stress regulation show promise, but broader systemic change remains essential.
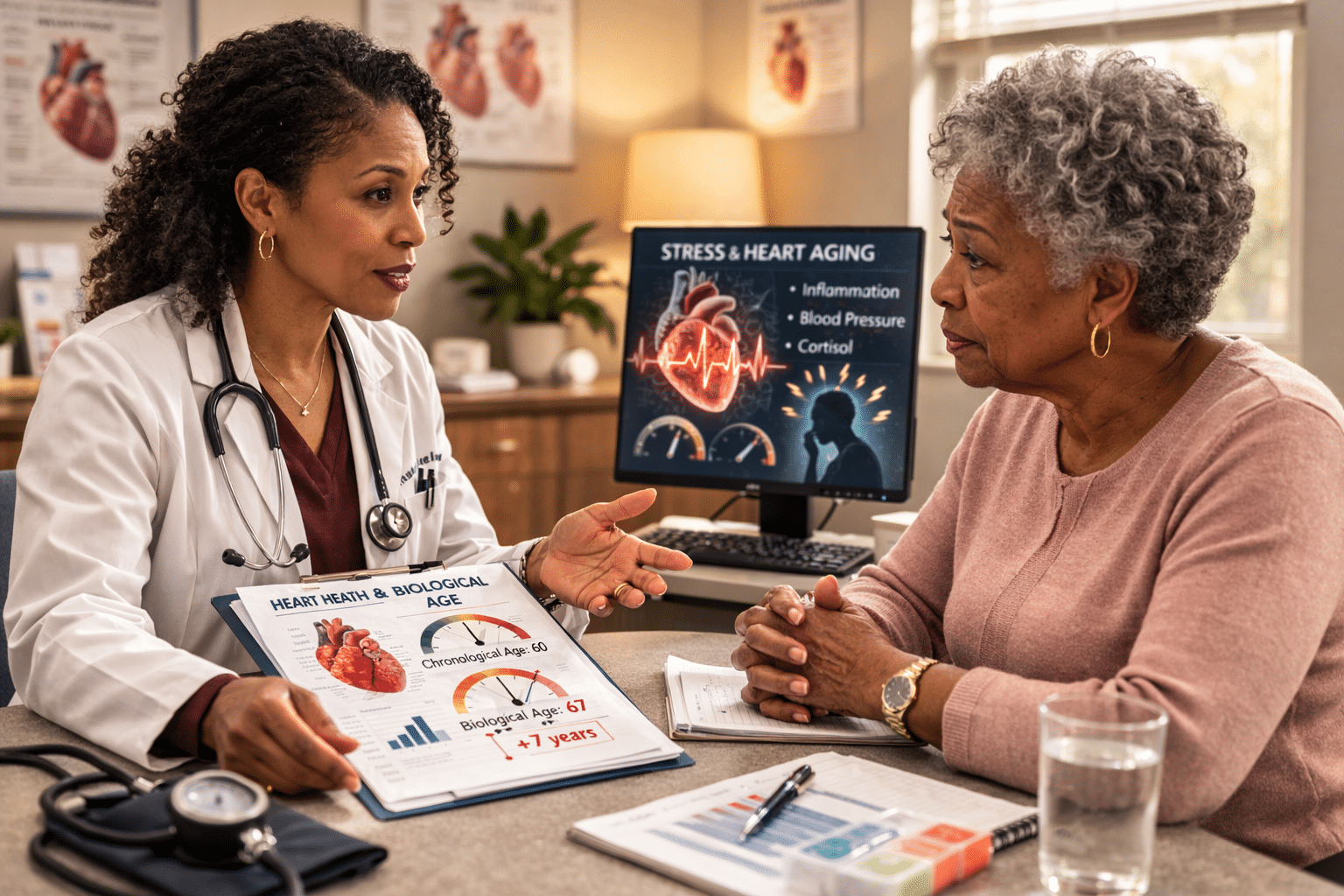
How Can Healthcare Providers Look Beyond Age?
For healthcare providers, the weathering framework should prompt questions to determine whether these societal factors are present, even when a patient hasn’t yet linked their circumstances to their health. Incorporating discussions of stress exposure, environmental strain, and inflammatory risk factors into wellness visits may allow earlier detection of cardiovascular disease.
Similarly, care providers shouldn’t rely solely on patients’ self-reported symptoms; blood, stress, and hormone tests may be more definitive. When Black patients, especially young and female ones, present with borderline labs or subtle symptoms, clinicians should consider the cumulative stress burden that traditional calculators do not capture.
To be clear, weathering is not about defining race biologically. Instead, it is about recognizing how lived experience shapes physiology. Acknowledging the phenomenon can help patients and providers get on the same page early about the need for consistent cardiovascular care, even at younger age ranges.
