
Asymptomatic, average-risk women aged 50 to 74 years should receive biennial screening for breast cancer, according to a guidance statement published online April 17 in the Annals of Internal Medicine to coincide with the Internal Medicine Meeting, the annual meeting of the American College of Physicians, held from April 16 to 18 in San Francisco.
Amir Qaseem, M.D., Ph.D., from the American College of Physicians in Philadelphia, and colleagues present updated guidance for internal medicine physicians and other clinicians on screening asymptomatic, average-risk adult women for breast cancer.
According to the guidance, clinicians should discuss the risk for breast cancer, values and preferences, and uncertainty surrounding benefits and harms of screening for breast cancer in asymptomatic, average-risk women aged 40 to 49 years; if women in this population prefer to get screened, clinicians should initiate screening mammography every two years following shared decision-making. Clinicians should use biennial mammography for breast cancer screening for asymptomatic, average-risk women aged 50 to 74 years. Clinicians should discuss discontinuation of breast cancer screening based on shared decision-making in asymptomatic, average-risk women aged 75 years or older, or asymptomatic average-risk women with a limited life expectancy. Clinicians should consider using supplemental digital breast tomosynthesis for asymptomatic, average-risk adult women with breast density of Breast Imaging Reporting and Data System category C or D; supplemental magnetic resonance imaging or ultrasound should not be used for these women.
More breast cancer screening studies “are needed to evaluate the accuracy of different modalities, the benefits and harms of screening intervals, and adult females with dense breasts, particularly those receiving supplemental screening,” the authors write.
In response to the updated guidance statement, the American College of Radiology and Society of Breast Imaging stressed that women should start annual screening at age 40 years. “New American College of Physicians breast cancer screening guidelines rely on outdated and hyperbolic information, will cause continued confusion among women, and may contribute to thousands of additional breast cancer deaths each year,” the organizations write in a statement.
“Thousands more women would endure extensive surgery, mastectomies, and chemotherapy for advanced cancers than if their cancers were found early by an annual mammogram.”
The updated ACP recommendations state that women aged 50 to 74 should receive biennial mammography, while shared decision-making is advised for women aged 40 to 49.
For Black women, who are more likely to be diagnosed with early-onset breast cancer before age 50, following these recommendations may contribute to delayed detection in some patients. Black women have a higher incidence of breast cancer before age 40 and a 41 percent higher mortality rate than white women. They are also more likely to develop aggressive, advanced-stage, and triple-negative breast cancers.
While the ACP recommends shared decision-making for breast cancer screening at age 40, Black women may benefit from earlier individualized risk assessment in their mid-to-late 30s.
Several barriers to care contribute to breast cancer disparities among Black women, including delayed follow-up care, treatment inequities, insurance coverage gaps, and structural racism.
For breast cancer screening specifically, research shows that misconceptions about mammograms, fear of diagnosis, and limited access to care may prevent some Black women from receiving recommended preventive services.
To improve care delivery and patient outcomes, primary care providers and OB-GYNs should prioritize timely navigation, screening access, and diagnostic follow-up for Black women approaching screening age.
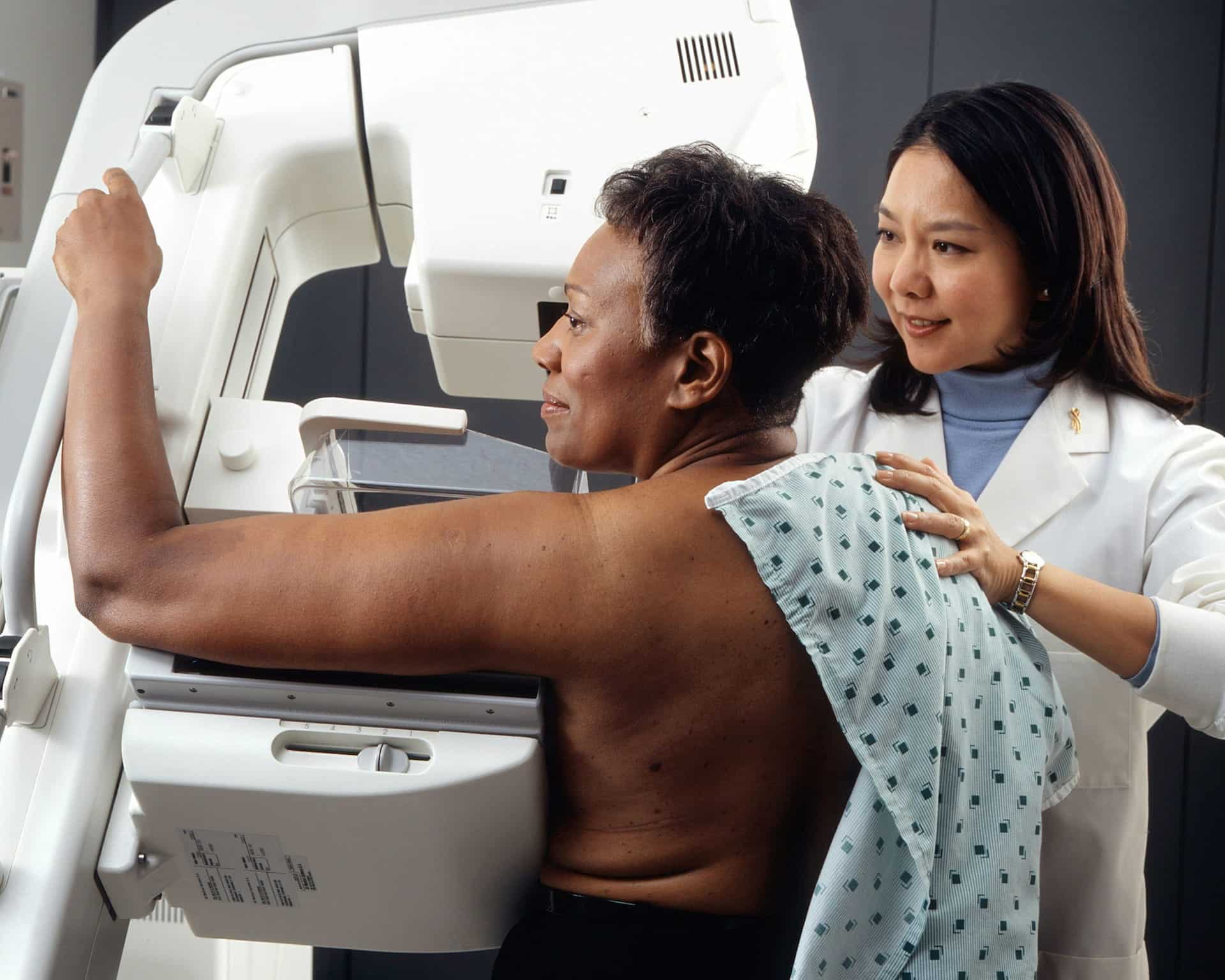
Because Black women are more likely to develop breast cancer at younger ages than other racial or ethnic groups, clinicians may need to consider individualized risk assessment strategies to support early detection.
Providers should assess patients for factors such as:
Clinicians should also consider discussing the American College of Radiology’s (ACR) breast cancer screening guidance, which recommends annual mammograms beginning at age 40 for women at average risk.
The ACP emphasizes shared decision-making between providers and patients — and this can be especially important when caring for Black patients.
Certain barriers can make it challenging for Black patients to get compassionate, high-quality healthcare, including:
To encourage Black women to get annual mammographies at age 40 or earlier, it’s on providers to ensure they deliver compassionate and culturally responsive communication and care to change patient behaviors.
Providers can take the following actionable steps to improve preventive breast cancer care for Black women:
By subscribing, you consent to receive emails from BlackDoctor.pro You may unsubscribe at any time. Privacy Policy & Terms of Service.
Are you a healthcare professional? Register with us today!